Vaginal infections and vaginitis—an umbrella term for inflammation of the vagina—are extremely common, and most women will experience at least one episode during their lifetime, often more than once. Typical symptoms include changes in vaginal discharge, itching, burning, pain or discomfort, and a noticeable odor. While some infections are sexually transmitted, many of the most frequent causes are not.
Why vaginal infections happen
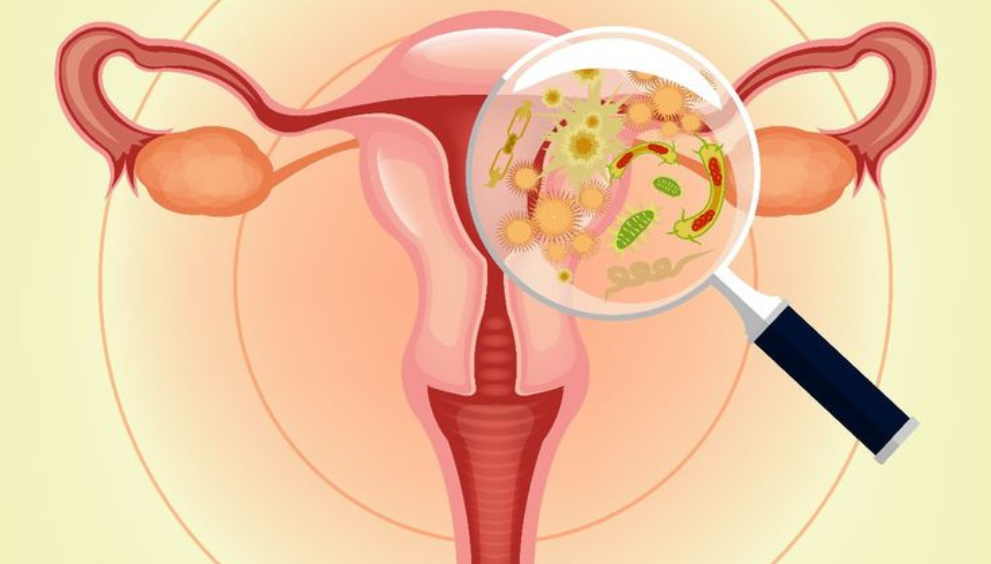
The vagina hosts a complex microbiome—mainly Lactobacillus species—that helps maintain a slightly acidic pH and keeps potential pathogens in check. When this balance is disrupted, bacteria or yeast can overgrow and trigger symptoms. Common disruptors include:
- Douching or internal rinsing with liquids
- Shifts in estrogen and other hormones (e.g., pregnancy, postpartum, menopause)
- Recent antibiotic use
- Vaginal intercourse and new sexual partners
- Breastfeeding-related low estrogen
Note: Douching is unnecessary and can be harmful because it disturbs the natural flora and pH.
Find professional companionship services, offering trusted options, With services centered around a Call Girl in Koti, you can also explore reliable and confidential choices for a Call Girl in Kokapet within the same seamless experience.
The three most common causes
According to clinicians, the majority of symptomatic vaginitis cases fall into one of three categories: yeast infections, bacterial vaginosis (BV), or trichomoniasis. Each has hallmark features and specific treatments.
Yeast infection (vulvovaginal candidiasis)
A yeast infection arises when Candida—most often Candida albicans—overgrows in the vagina. Candida normally lives on the skin and mucosa without causing problems, but certain conditions tilt the balance toward overgrowth. Triggers include hormonal shifts related to pregnancy, birth control, menstruation, or menopause; persistent high blood sugar; and immune suppression due to medical conditions. Symptoms commonly include intense itching, irritation, and a thick, white discharge often likened to cottage cheese. Over-the-counter antifungal treatments (creams, ointments, suppositories) can help with straightforward cases, while recurrent, severe, or atypical presentations may require prescription therapy and confirmation of the yeast species.
Bacterial vaginosis (BV)
BV occurs when protective Lactobacillus levels drop and are replaced by mixed anaerobic bacteria, frequently including Gardnerella. BV often produces a thin, gray-white or clear, slippery discharge and a fishy odor that may be more noticeable after sex; itching and burning are less prominent than with yeast. Standard treatments include antibiotics such as metronidazole or clindamycin, available as oral tablets or as vaginal gels/creams. Many cases resolve with a single course, but recurrences are common and sometimes need retreatment or maintenance strategies. Because BV is associated with a higher risk of certain STIs and pregnancy complications, timely diagnosis and appropriate care matter.
Trichomoniasis
Trichomoniasis (“trich”) is a true sexually transmitted infection caused by the parasite Trichomonas vaginalis. Symptoms overlap with other causes—burning, irritation, redness, swelling, and pain with urination or sex—and the discharge may be yellow-gray or greenish with a strong odor. Diagnosis is typically confirmed with lab testing. Treatment involves prescription antibiotics effective against parasites, often given as a single large dose or a short multi-dose course. Sexual partners should be treated, and sex should be avoided until treatment is complete and symptoms have resolved.
Other conditions that can affect the vagina
Chlamydia
Chlamydia is a sexually transmitted infection that can cause inflammation in the cervix and the upper part of the reproductive system. Some individuals have discharge, while others have no symptoms at all. If the infection spreads, spotting between periods or bleeding after sex can occur, but bleeding has many possible causes, so evaluation is important. Routine screening is recommended for sexually active younger individuals because silent infections can threaten fertility. Treatment involves antibiotics, and partners should be evaluated and treated as indicated.
Gonorrhea
Gonorrhea is another highly contagious STI that may present with discharge, painful urination, or discomfort during sex—or no symptoms at all. Co-infection with chlamydia is common, so a positive test for one often leads clinicians to treat for both. Timely antibiotic treatment and partner management are essential to prevent complications.
Noninfectious vaginitis
Not all irritation is infectious. Noninfectious vaginitis stems from irritation or allergic reactions to products like scented tampons, fragranced soaps, fabric softeners, vaginal sprays, or douches. First steps include removing the suspected irritant and simplifying hygiene. In more stubborn cases, short courses of topical medications may be used under medical guidance.
Atrophic (genitourinary syndrome of menopause)
Falling estrogen around menopause—or during lactation—can thin and dry the vaginal tissues, causing burning, irritation, and pain with intercourse. Options include regular use of vaginal moisturizers and lubricants, and for appropriate candidates, clinician-prescribed local estrogen therapy.
Vulvodynia
Vulvodynia is chronic vulvar pain without a clear cause. It can feel like burning, stinging, rawness, or soreness and may be constant or triggered (e.g., by touch). Management is individualized and can include pelvic floor therapy, topical treatments, systemic medications, and behavioral strategies, often coordinated by a specialist.
Viral causes
Viruses, primarily herpes simplex virus (HSV), can cause painful ulcers or sores on the vulva and vaginal tissues. Lesions may be visible externally, but deeper infections require a pelvic exam and testing for confirmation. Antiviral medications can reduce outbreak severity and frequency, though HSV is a chronic, manageable condition rather than curable.
When to see a clinician
Because symptoms overlap widely across causes, self-diagnosis is unreliable. Seek care for:
- New, persistent, or recurrent discharge, itching, burning, odor, or pain
- Bleeding after sex or between periods
- Painful urination or pelvic pain
- Visible sores or lesions
- Fever or systemic symptoms
- Possible STI exposure or a new sexual partner
- Symptoms during pregnancy
Prompt evaluation ensures the right test, the right treatment, and fewer complications. Completing prescribed therapies, abstaining from sex when advised, and ensuring partners are treated (for STIs) are critical steps toward full resolution and prevention of reinfection.
Practical prevention tips
- Avoid douching and fragranced products; clean the vulva with lukewarm water and a gentle, unscented cleanser only on the outside.
- Wear breathable underwear and change out of damp clothes promptly.
- Use adequate lubrication during sex; consider condoms and barrier methods compatible with sensitive skin.
- If antibiotics are needed for any condition, consider discussing probiotic support with a clinician.
- Manage blood sugar if living with diabetes, as high glucose favors yeast overgrowth.
- Seek routine sexual health screening as recommended for age and risk.
Key takeaways
Vaginal infections and vaginitis are common and often manageable with accurate diagnosis and targeted treatment. Because symptoms can look alike across yeast, BV, trichomoniasis, STIs, and noninfectious causes, professional evaluation is the safest path. Reducing irritants, supporting the vaginal microbiome, practicing safer sex, and finishing prescribed treatments can minimize recurrences and protect long-term reproductive health.
FAQs
- What is vaginitis?
Vaginitis is an infection or inflammation of the vagina that may lead to unusual discharge, itching, burning, unpleasant odor, pain while urinating, or discomfort during intercourse. It has multiple causes, including bacterial vaginosis, yeast infections, trichomoniasis, irritant/allergic reactions, skin disorders, and low estrogen. - How do symptoms differ between yeast infection, BV, and trichomoniasis?
Yeast infections typically cause intense itching and thick, white “cottage cheese” discharge; BV often causes thin gray-white discharge with a fishy odor (especially after sex) and little itching; trichomoniasis may cause yellow-green or gray, sometimes frothy discharge with odor, plus burning or irritation. - Can vaginitis occur without a sexually transmitted infection?
Yes. BV and yeast infections commonly occur without sexual transmission. Irritant/allergic reactions and low-estrogen atrophy also cause vaginitis without being STIs. - What are the most reliable signs I should get tested instead of self-treating?
New or persistent symptoms, strong odor, unusual discharge color/texture, pain with sex or urination, spotting between periods, pelvic pain, sores or blisters, fever, symptoms during pregnancy, or recurrent episodes all warrant clinical testing rather than self-treatment. - Is douching helpful or harmful?
Harmful. Douching disrupts the natural balance of vaginal flora and pH, increasing the risk of infections and irritation. - Can antibiotics cause vaginitis?
Yes. Antibiotics can reduce protective bacteria, making yeast overgrowth more likely and sometimes contributing to BV recurrences. - How is vaginitis diagnosed?
A clinician reviews symptoms and history, performs a pelvic exam if indicated, and tests a sample of vaginal discharge (and often urine or STI tests) to identify the specific cause. Accurate diagnosis is key because treatments differ.