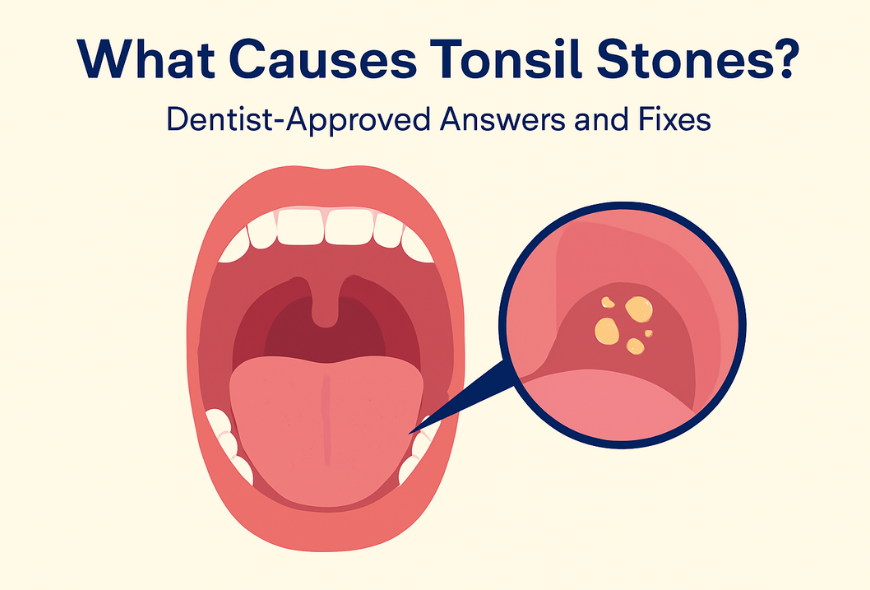
If you often sense a weird lump at the back of your throat, or battle relentless bad breath that brushing can’t fix, you may have a tonsil stone. These hardened deposits, also called tonsilloliths, often hide within the crypts (deep folds) of your tonsils. While many small ones go unnoticed, some lead to discomfort, odor, or throat irritation.
In this article, you’ll get dentist-approved answers: what causes tonsil stones, how they develop (including tonsillar concretions and tonsil calcifications), and how to remove or minimize them safely. You’ll also find practical prevention steps, when to see a professional, and real-world risks. By the end, you’ll be empowered with actionable solutions—not just vague suggestions. Let’s dive in.
What Is a Tonsil Stone (Tonsillolith)?
A tonsil stone (also called a tonsillolith) is a small, hardened accumulation of debris (food particles, cellular debris, bacteria) that becomes calcified in the recesses of the tonsils.
- These deposits are also referred to as tonsillar concretions or tonsil calcifications in medical and dental literature.
- Most people with tonsil stones are unaware of them—small ones seldom cause symptoms.
- A few grow large enough to trigger discomfort, bad breath, or visible lumps you can see in the back of your throat.
Because tonsil stones often harbor bacterial biofilms and produce sulfur compounds, they are a common cause of halitosis (bad breath) that doesn’t go away with brushing.
Why Do Tonsil Stones Form? (Dentist-Approved Causes)
Understanding the root causes of tonsil stones helps you tackle them better. Here are the main factors:
1. Deep or Enlarged Tonsillar Crypts
Your tonsils are not smooth surfaces; they have pits, folds, or crevices called crypts. In some people, these crypts are deeper or more irregular, providing places debris can lodge. Over time, that debris calcifies and becomes a stone.
Frequent inflammation or prior infections (tonsillitis) can further deepen or scar these crypts, making future stone formation more likely.
2. Accumulation of Debris: Food, Mucus, & Dead Cells
Tiny food particles, sloughed-off epithelial cells (dead skin inside the throat), mucus, and saliva can accumulate in those crypts. Inadequate clearance leads to build-up.
3. Bacterial Biofilms & Mineralization
Once debris is trapped, bacteria colonize it, forming a biofilm. Some bacteria produce enzymes and volatile sulfur compounds. Over time, minerals (mainly calcium salts) deposit, turning soft debris into hardened tonsil calcifications.
These biofilms also make stones more resistant to simple removal or dissolution.
4. Chronic Inflammation & Infection (Tonsillitis)
Repeated bouts of tonsil inflammation or infection can predispose you to stones. Inflammation widens crypts, increases secretions, and triggers more debris accumulation.
Some case studies specifically tie recurrent tonsillitis to the development of multiple or large tonsilloliths.
5. Dry Mouth, Mouth Breathing & Reduced Saliva Flow
Saliva helps flush debris and reduce bacteria load. If mouth breathing (especially during sleep) dries out your throat, or if certain medications (antihistamines, decongestants) reduce saliva, debris clearance suffers, increasing risk.
6. Sinus / Postnasal Drip & Mucus Overproduction
If you have chronic sinus drainage or postnasal drip, the extra mucus can deposit onto tonsils and mix with debris. That additional substrate helps feed bacterial growth.
7. Weak Immune Response / Microbial Imbalance
Some evidence suggests that immunocompromised patients may form stones at a higher rate, because they cannot manage bacterial overgrowth and debris as efficiently.
8. Diet & Lifestyle Factors
- Diets high in sugar can feed bacteria.
- Smoking or vaping irritates tonsils and may worsen crypt inflammation.
- Poor oral hygiene promotes more debris and bacterial load.
Taken together, these causes explain how tonsillar concretions and tonsilloliths develop. In short: deep crypts + trapped debris + bacterial colonization + mineral deposits = tonsil stone.
Common Symptoms & Risks of Tonsil Stones
Many tonsil stones cause no symptoms and remain undiagnosed. But when they grow or irritate surrounding tissue, you may notice:
- Persistent bad breath (halitosis) — often the first and most troubling sign.
- Bad taste or metallic flavor in the mouth.
- Sore throat, irritation, or scratchy sensation
- Foreign-body sensation (feeling like something is stuck in your throat)
- Difficulty swallowing (dysphagia), especially if a stone is large or pressing on surrounding tissue.
- Ear pain or referred pain — even if the stone does not contact the ear, shared nerve pathways may cause discomfort there.
- Cough or throat clearing triggered by irritation
- Tonsil swelling or inflammation, sometimes with redness
- In rare, extreme cases, large tonsilloliths have been mistaken for tumors or caused difficulty breathing.
Risks & complications:
- Repeated irritation can lead to local infection
- Chronic inflammation may worsen crypt anatomy
- Overzealous self-removal attempts may damage tonsil tissue, cause bleeding or infection
- For giant stones, misdiagnosis with tumors or abscesses in imaging is possible.
How Dentists & ENT Specialists View & Treat Tonsil Stones
Although ENT (ear, nose, throat) specialists typically manage tonsil stones, dentists often play a diagnostic role and sometimes assist in removal if the stone is accessible.
Dentist’s Role in Tonsil Stone Cases
- Detection during routine exams — dentists may spot visible stones or signs of chronic inflammation in the throat.
- Simple manual removal for small, superficial stones with gauze or specialized (soft) instruments. The dentist may advise care to avoid tissue damage.
- Referral — for deeper, recurrent, or symptomatic stones, dentists refer to ENT for advanced removal or further evaluation.
However, a dentist must be cautious. Aggressive removal attempts may irritate or even tear tonsillar tissue, causing bleeding or pushing stones deeper.
ENT / Specialist Approaches
ENT specialists have access to more tools and may use:
- Manual curettage / dislodging under local anesthesia
- Laser cryptolysis / RF ablation / coagulation — to smooth or shrink crypts, reducing areas where stones form.
- Coblation or cold-instrument crypt reduction
- Tonsillectomy or partial tonsil removal in severe, recurrent, or symptomatic cases to eliminate the substrate entirely.
Specialists make decisions based on symptoms, stone frequency, size, and impact on quality of life. They weigh benefits and risks. Tonsillectomy is not taken lightly, given the role of tonsils in immunity.
7 Dentist-Approved Fixes & Removal Methods
Below is a practical, progressive approach you can try (safely) for removal or mitigation of tonsil stones. If you ever feel pain, bleeding, or difficulty breathing/swallowing, stop and consult a professional.
- Gentle Saltwater Gargles
- Mix about ½ to 1 teaspoon of non-iodized salt in a glass (8–10 oz) of warm water
- Gargle for 15–30 seconds, several times daily
- Helps dislodge loose debris and reduces bacterial load in crypts. Many ENT and dental sources recommend this as a first-line remedy.
- Mix about ½ to 1 teaspoon of non-iodized salt in a glass (8–10 oz) of warm water
- Use a Low-Pressure Oral Irrigator / Water Flosser
- Direct a gentle, low-pressure stream toward the crypts to flush out stones
- Avoid high-pressure settings, which may injure sensitive tissue
- Many patients report success with water picks for small stones.
- Direct a gentle, low-pressure stream toward the crypts to flush out stones
- Manual Removal (Cotton Swab or Soft Tool)
- Use a moistened cotton swab or a soft silicone tip
- Gently press behind the stone (toward throat) rather than pushing against the tonsil surface
- Be cautious: avoid sharp objects, sudden pressure, or deep pokes
- This method works only if the stone is close to the surface and visible.
- Use a moistened cotton swab or a soft silicone tip
- Controlled Coughing / Throat Vibrations
- Forceful coughing can jostle stones loose
- Some also use sounds (like a guttural “k” or “g”) to vibrate tonsils, potentially dislodging hidden stones
- Forceful coughing can jostle stones loose
- Oral Rinses & Mouthwashes
- Use non-alcoholic, gentle antiseptic mouthwashes to reduce bacterial load
- Some formulas contain chlorhexidine or cetylpyridinium chloride, which may help suppress biofilm formation
- Use non-alcoholic, gentle antiseptic mouthwashes to reduce bacterial load
- Laser / Crypt Reduction Procedures
- For recurrent or stubborn stones, a specialist can perform laser cryptolysis to smooth or shrink crypts, reducing the “nooks” where stones form
- This is more invasive but may reduce recurrence over time.
- For recurrent or stubborn stones, a specialist can perform laser cryptolysis to smooth or shrink crypts, reducing the “nooks” where stones form
- Tonsillectomy (Last-Resort Option)
- If stones are large, highly symptomatic, and recurring, full or partial tonsil removal may be considered
- Removes the anatomical substrate, thus eliminating stones entirely—but comes with surgical risks.
- If stones are large, highly symptomatic, and recurring, full or partial tonsil removal may be considered
How to Choose the Right Approach (Step-by-Step)
Here’s a logical decision path you can follow to decide which fix is most appropriate:
- Assess symptoms & severity
- Are the stones causing bad breath, irritation, or swallowing trouble?
- Or are they asymptomatic?
- Are the stones causing bad breath, irritation, or swallowing trouble?
- Start with gentle, low-risk methods (gargling, oral irrigator)
- Try these for 1–2 weeks and monitor any changes
- Try these for 1–2 weeks and monitor any changes
- Attempt manual removal only when safe
- If the stone is visible, shallow, and easily accessible
- Stop immediately if pain or bleeding occurs
- If the stone is visible, shallow, and easily accessible
- See a dentist / ENT if no improvement or worsening
- Particularly if stones recur, grow, or cause persistent symptoms
- Particularly if stones recur, grow, or cause persistent symptoms
- Consider surgical / procedural intervention only when necessary
- After weighing risks, benefits, and alternatives
- Use partial approaches (e.g. crypt reduction) before full tonsillectomy
- After weighing risks, benefits, and alternatives
Preventing Tonsil Stones: Pro Tips
Preventive measures are often the best long-term strategy to reduce recurrence.
- Maintain excellent oral hygiene
- Brush twice daily, including the tongue
- Floss daily
- Use an antiseptic mouthwash if tolerated
- Brush twice daily, including the tongue
- Stay well hydrated
- Adequate saliva flow helps flush debris
- Avoid drying agents, excessive caffeine, or mouth breathing
- Adequate saliva flow helps flush debris
- Limit sugary, sticky foods and dairy
- These encourage bacterial growth
- These encourage bacterial growth
- Reduce mucus production / manage postnasal drip
- Treat allergies or sinus issues
- Use nasal saline rinses or antihistamines when needed
- Treat allergies or sinus issues
- Avoid smoking / vaping
- Reduces tonsil irritation and inflammation
- Reduces tonsil irritation and inflammation
- Regular gargling (e.g. after meals or before bed)
- Helps dislodge particles before they embed
- Helps dislodge particles before they embed
- Periodic throat self-inspection
- Use a flashlight and mirror to check for visible stones
- Removing small ones early is easier
- Use a flashlight and mirror to check for visible stones
- Sleep posture & breathing habits
- Try to reduce mouth breathing; use humidifiers or nasal strips
Even though no preventive strategy is fail-safe, combining many of the above reduces risk significantly.
Pitfalls, Misconceptions, and Warnings
- Don’t use sharp, pointed objects: Q-tips, toothpicks, or needles can tear tonsil tissue, cause bleeding, or push stones deeper.
- Not all throat lumps are tonsil stones: Some may be abscesses, tumors, or swollen lymph nodes. Always consult when in doubt.
- Gargling too aggressively may irritate tissue; moderate is safer
- High-pressure irrigators can damage soft tissue—use only low settings
- Surgery has trade-offs: Tonsillectomy carries risks (bleeding, pain, potential immune implications). The decision must be deliberate.
- Recurrence is possible: Even after removal, crypts remain unless modified
- Overdiagnosis on imaging: Not all calcifications in the tonsil area are harmful; some are incidental findings.
Mini Summary: Why Tonsil Stones Happen & What You Can Do
- Tonsil stones (tonsilloliths / tonsillar concretions) form when debris gets trapped in tonsil crypts and calcifies over time.
- Key contributors: deep crypts, chronic inflammation, bacterial biofilms, poor saliva flow, mucus, poor hygiene.
- Symptoms include bad breath, throat irritation, swallowing trouble, and ear pain.
- Start with gentle removal: gargling, irrigation, manual dislodging (carefully).
- For stubborn or recurrent cases, consult dentist or ENT for procedures like laser cryptolysis or tonsillectomy.
- Prevent recurrence by maintaining oral hygiene, hydration, limiting mucus, and managing sinus issues.
When to See a Professional / ENT
Seek medical evaluation if:
- You experience pain, swelling, or fever
- You can’t swallow or have breathing difficulty
- The stone recurs frequently (weekly, monthly)
- Removal attempts cause bleeding or worsening symptoms
- Imaging reveals large, unexplained masses
- Bad breath persists despite good oral hygiene
An ENT may perform imaging, scope examinations, or surgical removal based on findings.
Case Note (Illustrative Example)
Patient A is a 28-year-old who complained of chronic halitosis. Dentists found a 3 mm white nodule in the left tonsil crypt. Over two weeks, the patient used saltwater gargles 3× daily and a low-pressure oral irrigator nightly. The stone dislodged within days; breath odor resolved. The patient continued preventive measures and reported no recurrence over 6 months.
This case illustrates how mild stones often yield to conservative measures when applied consistently.
Conclusion
Tonsil stones, or tonsilloliths, may sound alarming, but they are usually benign and manageable with care. The key lies in understanding what causes tonsil stones—from deep tonsillar crypts to bacterial activity—and addressing those root factors. Start with safe, conservative measures like saltwater gargles, oral irrigation, and gentle manual removal (only when obvious and accessible). If symptoms persist, seek a qualified dentist or ENT for further treatment.
Prevention is your best long-term ally: strong oral hygiene, hydration, controlling mucus, and avoiding irritants all help. While surgical options like crypt reduction or tonsillectomy exist, they’re reserved for the most persistent cases.
If you’re struggling with symptoms or recurrent stones, or if you’re unsure whether what you have is a tonsil stone, I strongly recommend scheduling an evaluation with an ENT—all the better for peace of mind and targeted treatment.
FAQs
Q1: What causes a tonsil stone to form in the first place?
A: Tonsil stones form when debris—food particles, dead cells, mucus—gets trapped in the crypts of your tonsils. Bacteria then colonize this debris, forming a biofilm. Over time, minerals (primarily calcium salts) deposit and harden, creating a tonsil stone (tonsillolith). Deep crypts, frequent inflammation, reduced saliva, and poor hygiene all increase the chance of formation.
Q2: Does a tonsil stone always cause bad breath?
A: Not always. Many tonsil stones are asymptomatic. However, when present, they are a frequent cause of tonsil stone bad breath, because bacteria in the stone produce volatile sulfur compounds. Even small stones near the surface can lead to noticeable odor.
Q3: Can a dentist remove a tonsil stone safely?
A: Yes — in certain cases. If a stone is superficial and easily accessible, a dentist may gently dislodge it using soft tools. However, deeper, recurrent, or hard-to-reach stones usually require ENT evaluation to safely remove them without damaging tissue.
Q4: How can I remove a tonsil stone at home?
A: Start with gentle saltwater gargles, use a low-pressure oral irrigator, or carefully try manual removal with a moistened cotton swab (only if the stone is easily visible). Avoid sharp tools. If these methods don’t work or cause discomfort, stop and consult a professional.
Q5: Will tonsil stones come back after removal?
A: They may. Because the anatomical crypt structure remains, new stones can form. That’s why preventive steps—good oral hygiene, hydration, managing mucus/sinus issues, avoiding irritants—are important to reduce recurrence.
Q6: When should I get a tonsillectomy for tonsil stones?
A: Surgery is a last-resort option. It may be considered when stones are large, highly symptomatic, recurrent despite conservative management, or significantly affecting quality of life. A specialist evaluates risks and benefits before recommending tonsillectomy or crypt reduction.
Q7: Are tonsil stones dangerous?
A: In most cases, no—they’re benign. But if left unmanaged, they can irritate tissue, lead to infection, or cause discomfort. Attempts to forcibly remove them without skill may injure your throat. Rarely, very large stones may mimic tumors, so medical evaluation is important when in doubt.